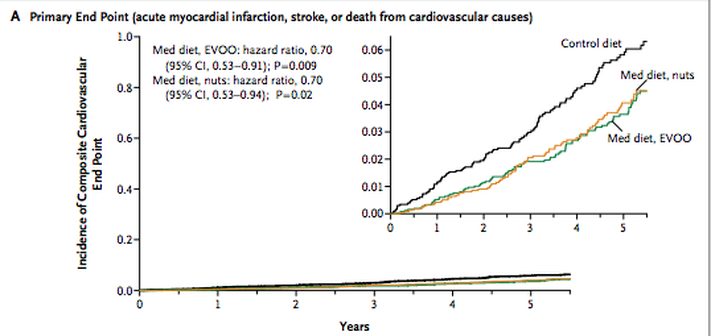
Many of you have probably already heard of this trial that just got published, an energy-unrestricted Mediterranean diet supplemented with either extra-virgin olive oil or nuts that resulted in an absolute risk reduction of approximately 3 major cardiovascular events per 1000 person-years, for a relative risk reduction of approximately 30%, among high risk persons who were initially free of cardiovascular disease, as compared to a control group consuming a typical low fat diet.
But you may not have heard Dr. Esselstyn's response. Dr Esselstyn is a successful surgeon (featured in video above) and author of “Prevent and Reverse Heart Disease: The Revolutionary, Scientifically Proven, Nutrition-Based Cure,” who promotes a low fat vegan diet that does not allow olive oil, dismissed the new study. Those in the Mediterranean diet study, he expained, still had heart attacks and strokes! So all the study showed was that “the Mediterranean diet and the horrible control diet were able to create disease in people who otherwise did not have it.”
This logic is absolutely absurd and needs to be addressed. The study population consisted of men and women with an average age of 67 (ranging from 55-80) with no cardiovascular disease at enrollment, who had "either type 2 diabetes mellitus or at least three of the following major risk factors: smoking, hypertension, elevated low-density lipoprotein cholesterol levels, low high-density lipoprotein cholesterol levels, overweight or obesity, or a family history of premature coronary heart disease."
In other words they were elderly patients followed for a median of 4.8 years, who were by definition at high risk to have a heart attack. So according to Dr. Esselstyn's logic, the patients would have been heart disease free during these 5 years had they not been enrolled in to this study and succumbed to the toxic effects of the mediterranean and "horrible control" diets that were able to actually "create disease" in the study subjects.
If this were true, then every randomized clinical trial in the history of medicine would be invalid, and ongoing trials must be stopped immediately due to ethical reasons and impending harm. A certain percentage of patients assigned to take a placebo in a drug trial will almost certainly develop the disease in question, as will many in the experimental group of even the most successful drug trials in history. Does this mean that the drug or placebo caused the diseases observed? Of course not. A successful drug would have prevented more disease or death than the placebo, but the disease still occurs in both groups.
And what was this "horrible control diet" he speaks of? Subjects in the control group were encouraged to eat low-fat dairy products, bread, potatoes, pasta, rice, fresh fruits, vegetables, lean fish and seafood, while avoiding foods such as vegetable oils, fried snacks, red meat, fatty fish, and visible fats in soups. Also known as the government recommended, low fat high carbohydrate diet.
As Gina Kolata reports in the New York Times, "The magnitude of the diet’s benefits startled experts. The study ended early, after almost five years, because the results were so clear it was considered unethical to continue."
Mrs. Kolata also says that these published findings were based on the first major clinical trial to measure the Mediterranean diet’s effect on heart risks. However, this is untrue. This result and early termination is almost identical to the last time the Mediterranean diet was tested to prevent heart disease, published in 1994 out of France.
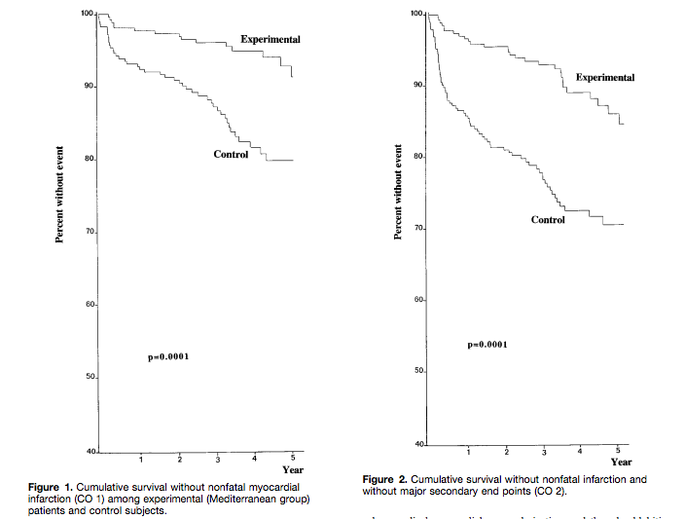
The Lyon Diet Heart Study, which tested the benefits of a Mediterranean-type diet on the recurrence of heart attacks in 605 subjects, was originally planned for five years but was ended prematurely due to the intervention diet’s dramatic cardio-protective effects. After 27 months, the risk of cardiac death or non-fatal MI was 73% lower in the experimental group compared to the controls (RR= 0.27, 95% CI: 0.12-0.59, p=0.0001) and overall mortality was 70% lower (RR=0.30, 95% CI: 0.11-0.82, p=0.02).
The benefits of the Mediterranean diet occurred despite no differences in serum LDL or total cholesterol levels between exposure groups, suggesting that diet’s influence on CVD risk extends further than the current, overly simplistic explanation that ties the mechanism to serum cholesterol elevations caused by excessive Saturated fat intake. At the four-year follow up, a 47% lower risk of CHD was experienced by the experimental group compared to the control group (RR=0.53, 95%CI: 0.38-0.74). There was a 72% decreased risk (RR=0.28, 95% CI: 0.15-0.53) of cardiac death and nonfatal MIs (14 events in the experimental group vs. 44 in the control, p=0.0001), and a 67% reduced risk (RR=0.33, 95% CI: 0.21-0.52) of secondary endpoints - unstable angina, stroke, heart failure, and pulmonary or peripheral embolism (27 events vs. 90, p=0.0001) - associated with the Mediterranean diet compared to the control diet.
Published in the Lancet in 1994, the Lyon study was originally rejected by the New England Journal of Medicine specifically because the intervention diet induced no changes in serum lipids, demonstrating how firmly held the diet-heart hypothesis was at the time, that somehow it was impossible to reduce heart disease without reducing total or LDL cholesterol.
When someone is confronted with inconvenient, overwhelming evidence contrary to their livelihood, it is understandably very difficult to concede. However, when the two most dramatic reductions in cardiovascular disease ever seen in clinical trial history are breathing down your neck, denial is the only possible escape.
Tried a paleo or low carb diet? Join Today and contribute to a better understanding of this way of eating!
View our Marketplace of paleo and low carb experts that compete against eachother to help you lose weight and get healthy!
 RSS Feed
RSS Feed
